Imagine your body as a busy highway, with drugs acting as vehicles navigating through. Sometimes, the journey is smooth, but at other times, traffic jams occur, leading to unexpected delays. This scenario is akin to pharmacokinetic drug interactions — a crucial aspect affecting how medications work in your body and their ultimate impact on your health. Whether you're someone taking multiple medications or curious about how drugs interact, this guide will shed light on the basics of pharmacokinetic drug interactions, their mechanisms, clinical implications, and how they can be managed effectively. You'll walk away with a stronger understanding of drug-drug interactions, metabolic drug interactions, and steps to minimize adverse effects.
Understanding Drug-Drug Interactions
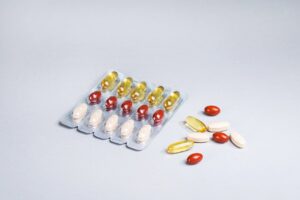 When two or more drugs are taken simultaneously, they can sometimes interact in ways that alter how your body processes them—this phenomenon is what we call drug-drug interactions. These interactions can either diminish the effectiveness of the medications or amplify their effects, potentially leading to adverse outcomes. For instance, taking a blood thinner like warfarin with certain antibiotics can increase the risk of bleeding, showcasing the critical nature of understanding these interactions. It's essential to communicate with healthcare professionals about all the medications you're taking, including over-the-counter drugs and herbal supplements. This step is pivotal in identifying potential interactions early on. Safe medication practices entail not only adherence to prescribed drug regimens but also an awareness of how drugs might interact with each other within your body.
When two or more drugs are taken simultaneously, they can sometimes interact in ways that alter how your body processes them—this phenomenon is what we call drug-drug interactions. These interactions can either diminish the effectiveness of the medications or amplify their effects, potentially leading to adverse outcomes. For instance, taking a blood thinner like warfarin with certain antibiotics can increase the risk of bleeding, showcasing the critical nature of understanding these interactions. It's essential to communicate with healthcare professionals about all the medications you're taking, including over-the-counter drugs and herbal supplements. This step is pivotal in identifying potential interactions early on. Safe medication practices entail not only adherence to prescribed drug regimens but also an awareness of how drugs might interact with each other within your body.
Decoding Metabolic Drug Interactions
Metabolic drug interactions occur when one drug affects the metabolism of another, typically within the liver, where most drug metabolism takes place. This can lead to either an acceleration or a slowdown in how quickly medications are broken down. For instance, if Drug A inhibits the enzyme responsible for metabolizing Drug B, levels of Drug B could rise, potentially leading to toxicity. Conversely, if Drug A accelerates the metabolism of Drug B, it might render Drug B less effective. Understanding these interactions is crucial, particularly for individuals on long-term medication regimes. To mitigate such risks, healthcare providers often adjust dosages or recommend alternative medications when metabolic drug interactions are anticipated. Being proactive in discussing all current medications with your healthcare provider can significantly help in managing these interactions effectively.
The What and How of Pharmacokinetic Interaction Mechanisms
 Pharmacokinetic interaction mechanisms delve into the intricacies of how drugs are absorbed, distributed, metabolized, and excreted by the body. These interactions can significantly influence the pharmacological effect of medications. For example, some drugs can compete for the same protein binding sites, leading to an increased concentration of one or both drugs in the bloodstream. Others may alter the pH level in the stomach, affecting the absorption rate of certain medications. Understanding these mechanisms is crucial for optimizing drug efficacy and minimizing adverse effects. Healthcare professionals often use this knowledge to tailor medication plans, ensuring that drugs with known pharmacokinetic interactions are carefully managed. Patients can support this process by consistently communicating their medication regimen and any changes to it.
Pharmacokinetic interaction mechanisms delve into the intricacies of how drugs are absorbed, distributed, metabolized, and excreted by the body. These interactions can significantly influence the pharmacological effect of medications. For example, some drugs can compete for the same protein binding sites, leading to an increased concentration of one or both drugs in the bloodstream. Others may alter the pH level in the stomach, affecting the absorption rate of certain medications. Understanding these mechanisms is crucial for optimizing drug efficacy and minimizing adverse effects. Healthcare professionals often use this knowledge to tailor medication plans, ensuring that drugs with known pharmacokinetic interactions are carefully managed. Patients can support this process by consistently communicating their medication regimen and any changes to it.
Managing Drug Interactions in Clinical Practice
 In clinical practice, managing drug interactions is a cornerstone of patient safety and effective medication management. This involves a comprehensive review of a patient's medication list, including prescription drugs, over-the-counter medications, and herbal supplements. Healthcare professionals leverage drug interaction checkers and clinical judgment to identify potential interactions and assess their clinical significance.
In clinical practice, managing drug interactions is a cornerstone of patient safety and effective medication management. This involves a comprehensive review of a patient's medication list, including prescription drugs, over-the-counter medications, and herbal supplements. Healthcare professionals leverage drug interaction checkers and clinical judgment to identify potential interactions and assess their clinical significance.
When interactions are identified, strategies such as adjusting the dosing schedule, substituting with alternative medications, or closely monitoring the patient for signs of adverse effects can be employed. Engaging patients in discussions about the importance of reporting all substances they're taking and any side effects experienced is crucial. Through this collaborative approach, the risk of significant drug interactions can be minimized, enhancing the overall efficacy of the treatment plan.
Tackling Adverse Effects of Drug Interactions
The adverse effects of drug interactions can range from mild to severe, impacting patient health and quality of life. These effects may manifest as unexpected side effects, reduced medication efficacy, or even dangerous health conditions. Awareness and early detection are key to preventing serious outcomes. Healthcare providers play a crucial role in educating patients about potential signs of adverse interactions and implementing preventive measures. Patients are encouraged to maintain open communication with their healthcare team, reporting any new symptoms or changes in their health. Regular medication reviews can also help in identifying and addressing potential drug interactions proactively. By staying informed and vigilant, both patients and healthcare providers can work together to tackle the adverse effects of drug interactions, ensuring safer and more effective treatment outcomes.
Practical Tips for Minimizing Drug Interaction Risks
 Minimizing the risks associated with drug interactions involves proactive measures and informed decision-making by both patients and healthcare professionals. Here are practical tips to keep in mind:
Minimizing the risks associated with drug interactions involves proactive measures and informed decision-making by both patients and healthcare professionals. Here are practical tips to keep in mind:
- Maintain an Up-to-Date Medication List: Include all prescription medications, over-the-counter drugs, supplements, and herbal products.
- Consult With Healthcare Providers Regularly: Before starting new medications, discuss potential interactions with your doctor or pharmacist.
- Use a Single Pharmacy: This can help ensure that all medication records are centralized, making it easier to monitor for interactions.
- Educate Yourself: Understand the purpose of each medication and be aware of common interactions related to your medications.
- Monitor for New Symptoms: Report any unexpected changes in your health to your healthcare provider promptly.
By applying these strategies, individuals can significantly reduce the risk of adverse drug interactions and promote safer medication use.
